Facility Facts
Understanding the Grant Application
Explaining Low-Barrier and General Concerns
A low-barrier homeless facility can raise concerns because it typically has minimal entry requirements. Often no proof of residence, no ID or background checks, and allowing individuals with criminal records. These facilities usually do not require sobriety and may serve individuals with untreated mental health or substance use issues, leading to fears about unpredictable behavior. Flexible, often 24/7 access can increase foot traffic at all hours, while fewer upfront behavioral requirements raise concerns about conduct before intervention. Allowing pets and personal belongings may add to worries about cleanliness and loitering, and because these facilities are more accessible, they may draw a larger, higher-need population, raising concerns about increased concentration and impacts on the surrounding area.
Target Population Concerns
When a facility serves a population where a significant percentage of residents are experiencing serious mental illness (57%) or substance use disorder (43%), it is reasonable for nearby residents to have concerns. These conditions can, at times, involve crisis episodes, impaired judgment, or unpredictable behavior, particularly if individuals are not required to be stabilized before entry. When combined with a model that allows residents to come and go freely, it can lead to increased foot traffic and activity around the site throughout the day, including during school hours.
Given the facility’s location a block from a middle school, it is valid for parents and neighbors to be concerned about student safety, exposure to disruptive or concerning behavior, and whether appropriate boundaries and supervision can be consistently maintained. Many residents also feel that public safety was not adequately considered in selecting this location, especially given the proximity to children and the nature of the population being served. These concerns are not about stigma, they reflect practical questions about proximity, population needs, and operational structure.
While outcomes depend heavily on management and safeguards, the combination of a high-needs population, fewer entry barriers, and a school-adjacent location makes this location deeply concerning.


Understanding the County Recorded Declaration of Restrictions
Medical Respite or Homeless Shelter?
The operator has described the facility as a “medical respite center,” but that characterization conflicts with the county-recorded document governing the property. While the label may sound reassuring, a closer reading of the actual agreement shows it offers little real protection for the community.
For starters, the document does not guarantee that only medical respite patients will live there. It explicitly allows the operator to house non-qualified residents if the intended population isn’t available. In other words, the facility could serve an entirely different population without violating the agreement.
Even more concerning, the restrictions are not permanent. The agreement allows changes with state approval, meaning the property could be repurposed at any time in the future, including as a larger homeless shelter, without meaningful local input.
The document cites 105 beds, but that number is far from a fixed limit. With 54 rooms and nearly 40,000 square feet, the facility could accommodate far more people depending on how it is configured. At moderate density (3–4 people per room), the site could house approximately 162–216 residents. Under a more intensive, congregate-style model (4–6 people per room, with potential use of common areas), capacity could reach 216–324 or more. In practice, physical capacity, not the stated bed count, determines how many people can be housed, and that capacity can increase over time.
Adding to the concern, this project was approved under California Assembly Bill 172, which bypassed local zoning rules and oversight. As a result, the city has limited authority over how the property is used or expanded. The state holds primary control over approvals, often with minimal public notice or input.
Many residents assume the “medical respite” label ensures hospital-like care. However, the recorded document does not actually define the facility that way. Instead, it is classified as an “adult and senior care facility”, a broader designation that allows for flexibility in how the site is used and who can be housed there.
Moreover, the intended population of SSI/CAPI recipients appears too small to fill the facility. With only about 130 unsheltered seniors (over age 55) in all of Placer County, the operator may rely on the provision allowing additional residents to reach capacity. In practice, this could result in the facility functioning more like a general homeless shelter than the narrowly defined program many residents expect.
In short, what may appear to be a safeguard is, in reality, a loosely defined agreement with significant flexibility. Both the use and scale of the facility can change at any time, and without clear, enforceable, and permanent restrictions, there is little to prevent outcomes the community may not have anticipated or supported.


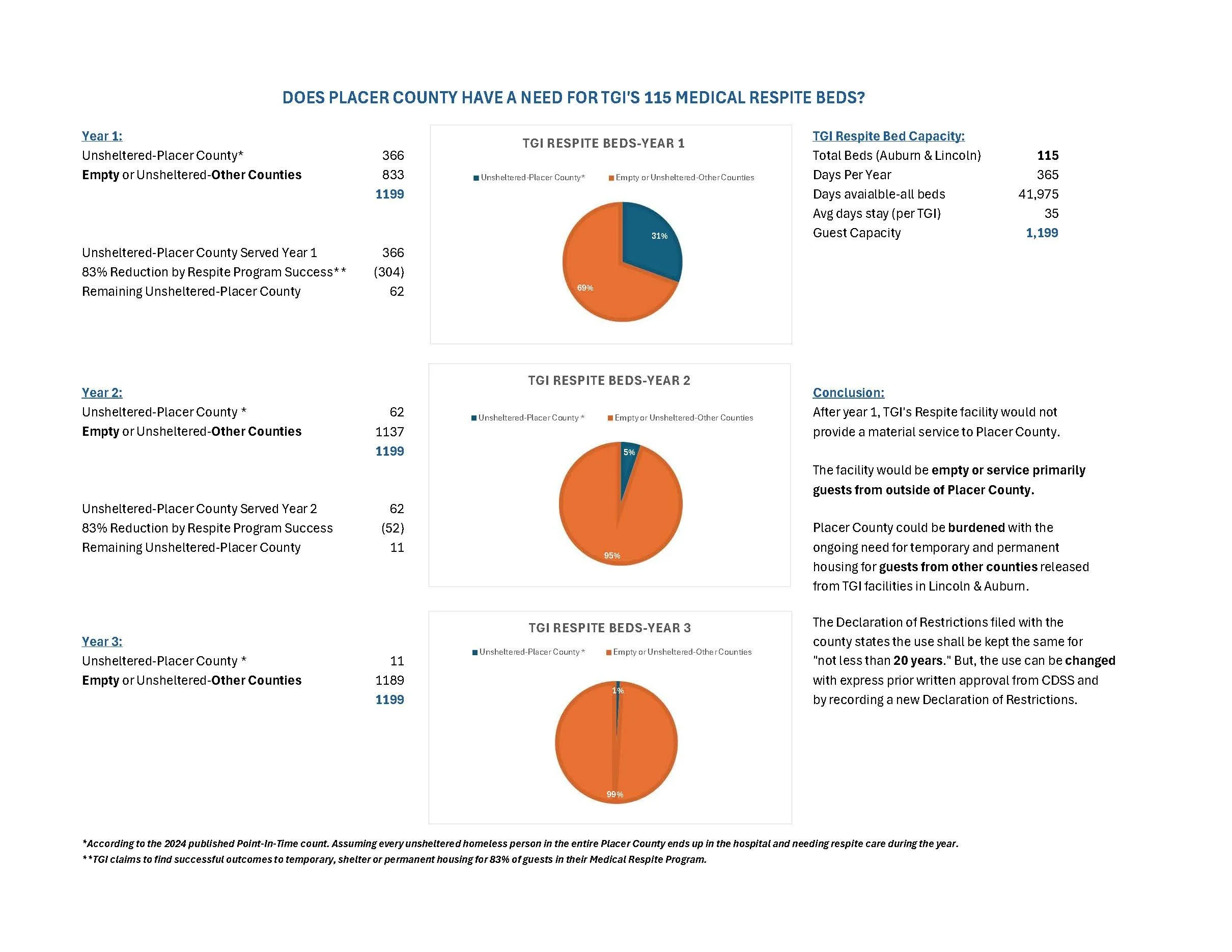
Will this only serve Placer County?
Will this impact EMS/Fire response times?
City of Lincoln Alleges Significant Impact
Based on documented data from a 10-bed medical respite facility in Auburn, where first responders handled 141 calls for service in a single year, the potential impact of a much larger facility becomes significant. That equates to roughly 14 calls per bed annually, meaning a proposed 105-bed facility in Lincoln could generate nearly 1,500 emergency calls per year, and if expanded to 300 beds or more, over 4,000 calls annually. For a city like Lincoln—with no city-based advanced life support ambulances, reliance on outside paramedic services, and hospital transport times often exceeding 25 minutes, this level of demand raises serious public safety concerns. For residents in Lincoln’s large senior communities, where emergencies such as heart attacks, strokes, and falls require immediate response, even small delays can have life-threatening consequences. When emergency units are tied up responding elsewhere, response times increase, and in those critical moments, every minute truly matters.
Primary Data Source
Legal complaint / project documentation referencing emergency service calls at an Auburn medical respite facility
Reported 2024 annual calls:
Cal Fire: 67 calls
Sheriff: 74 calls
Total: 141 calls at a 10-bed facility
Extrapolation Method
Calculated per-bed call rate:
141 calls ÷ 10 beds = 14.1 calls per bed per year
Applied linearly to proposed facility sizes:
105 beds → ~1,480 calls/year
300 beds → ~4,230 calls/year
Beyond emergency response strain, this level of service demand also carries a significant financial impact for the City of Lincoln. Police, fire, and administrative services are largely funded through the City’s General Fund, which supports core services residents rely on every day. A substantial increase in calls for service, potentially numbering in the thousands annually, would require additional staffing, overtime, equipment, and long-term infrastructure support. If these costs are not fully offset by the facility operator or external funding sources, the burden would fall on local taxpayers. Over time, this could mean well over $1 million annually in General Fund expenses, forcing difficult trade-offs between maintaining current service levels, funding new resources, or reallocating dollars away from other community priorities.
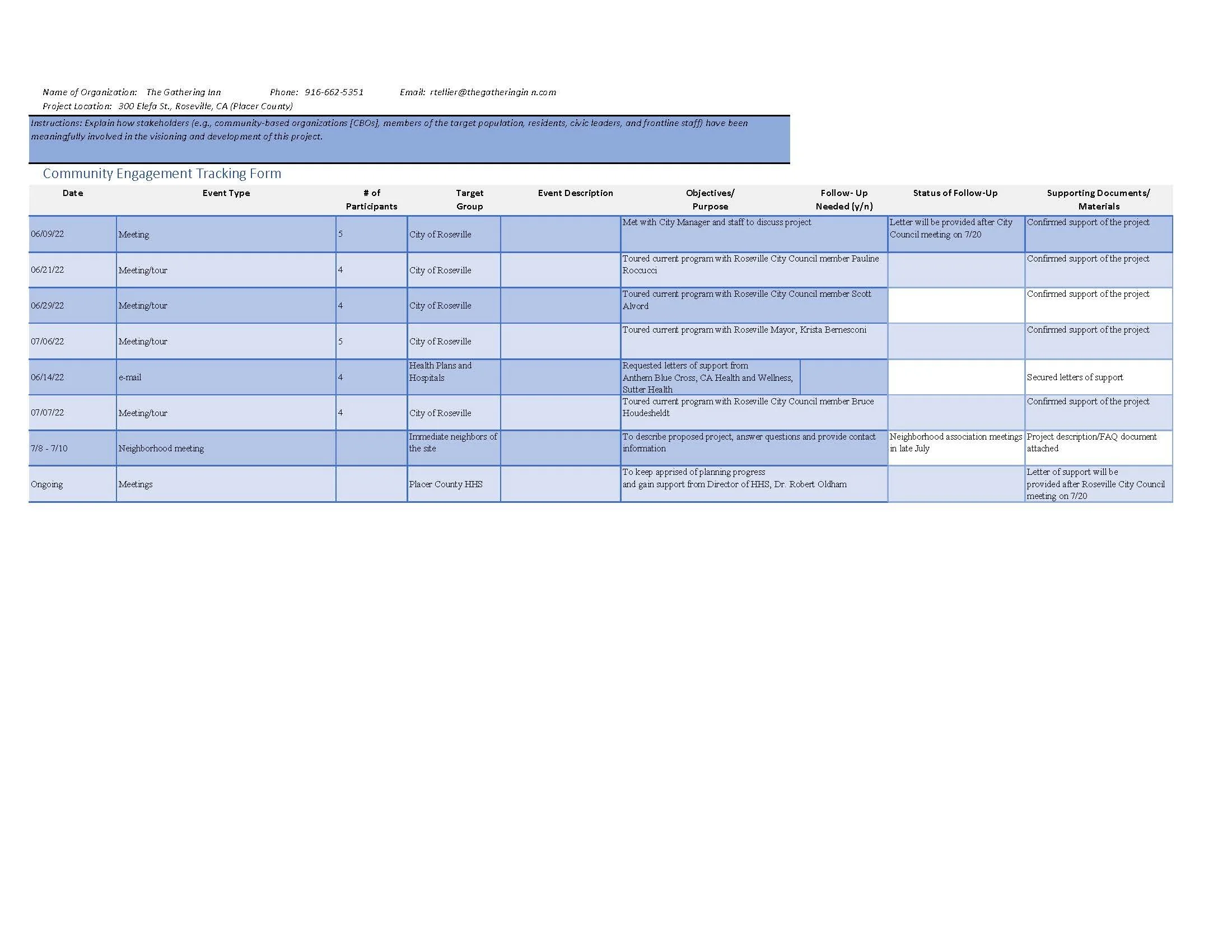
Community Outreach Submitted with Grant Application in September 2023 (None conducted with Lincoln Elected Officials or Residents)